Around
late October 2008, I was having coughing fits and actually was coughing up a
little
blood. Went to Solantic and they did a chest X-ray, but said it was okay, the
X-ray came back as “normal lung” (see examples at the bottom of this page). I indicated that it felt like I was gargling
blood high up in the throat area. The coughing of the blood was not constant,
off and on, but visited Solantic since if was after normal doctor office hours,
but not an emergency room since it was not “real bad”. (link:
http://en.wikipedia.org/wiki/Hemoptysis)
The following day I went to my primary doctor (although have yet to ever see Dr.
Prince, but rather say one of the PAs), gave her the same story. I asked if it
could be my lungs, and she said if it was, I would be in the emergency room
right now, so I figured it must not be anything to do with my lungs. She gave
me a referral for a upper GI scope to check out my throat/stomach/etc.
In November of 2008, I went through then endoscopy procedure to check out my GI
tract. That doctor said that I might have a small hiatus hernia and said to
make sure not to eat too late and then go to bed (lying down right away),
perhaps excess stomach acid was causing an issue. I agreed even though I had
never had any issues with indigestion, but I was 39 years old and things
change. He also issued me a proton-prohibitor medicine (a generic Protonix) to
help with excess acid build up. By mid-November it seemed to be fine. I only
took the Protonix for 30 days and made sure I did not eat anything a couple of
hours before bed/lying down.
Time passes, no more coughing up blood, no issues, I guessed it was something to
do with stomach/acid/etc.
In February of 2009 I got the flu pretty bad, but again no issues coughing up
blood, etc.
In 2009 I switched to a BCBS PPO plan at work. Katie had also read in the Wall
Street Journal that the Mayo Clinic (which has a facility right here in
Jacksonville) did something called an Executive Annual Physical program (link:
http://www.mayoclinic.org/executive-health). Mayo accepts BCBS PPO plan, so
with Katie’s suggestion, I set up an annual physical there in October of 2009.
I figured that would be a good thing to do since I was going to be turning 40
years old the following March and this would be a great baseline for my current
health.
Note: Click here for a
list of the items the did during my annual physical visit.
Mayo’s Executive Annual Physical includes a full checkup, blood work,
urinalysis, chest X-ray, EKG, body composition, and a tread-mill stress test.
And Mayo is an excellent place to go, so this was a great way to check out
where I was health wise. I had been slowly losing extra weight to help my
blood pressure and cholesterol levels, so this was just a next step as a
comprehensive baseline. I knew going in that some of the procedures were “not
covered or not full covered” under a normal annual physical, but I figured the
out-of-pocket expense was worth knowing.
So, on October 28th (Wednesday) I had my annual physical with Mayo.
The doctor, Dr. Manuel Rodriguez MD (link:
http://www.mayoclinic.org/bio/13483803.html), was the doctor doing my main
physical. Dr. Rodriguez was just the nicest doctor, explaining all of things he
was checking during the physical and really showing a kindness and concern for
his patient. After all of the tests and procedures I was to have a final
meeting with him and that is when he explained that my chest X-ray showed that
my upper right lobe was collapsed. Dr. Rodriguez’s concern and compassion was
very obvious, making sure to let me know not to worry and that they are going to
take good care of me. He even gave me his business card and added his personal
home/cell phone numbers so if Katie or I had any questions we could call him
directly.
They attempted to schedule me for CT scan that same day, but could not get the
authorization back from BCBS fast enough, so it was scheduled for the following
day, Thursday, October 29th.
Since I was able to leave the hospital about 2pm that day, I was
able to contact Solantic and get a copy of my chest X-ray from the prior year so
I could bring in to Dr. Rodriguez on Thursday for a comparison.
I went to the Mayo clinic early that morning for the CT scan, and meet with Dr.
Rodriguez that afternoon to discuss the findings. He showed me the CT scan
which revealed that there was something in the right upper bronchial tube
obstructing air flow. The scan showed that some air was able to get in there,
but not much. At this point it was unclear what t was, meaning it could be
mucus, a growth, or even possibly something I swallowed incorrectly
(bean/etc.). We also reviewed the chest X-ray from Solantic the prior year and
both X-rays looked almost the same. And as I heard from Dr. Rodriguez, this
was a “classic example of a collapsed lung”. So, apparently the radiologist
and/or doctor at Solantic completely missed it and said it was a normal lung.
One good thing from the comparison showed that for at least one year, the upper
right lobe of my lung was not functioning. They said that the upper right lobe
only provides about 18% of your air capacity, and that is why I probably never
felt any shortness of breath/etc.
The next step was to meet with pulmonary doctor. The next appoint that was
scheduled was not until around 3+ weeks later. Dr. Rodriguez called he doctor
on the schedule, a Dr. Jorge Pascual MD (link:
http://www.mayoclinic.org/bio/11203561.html) , to see if it was possible for
him to fit me in the next day, which would be incredible. Dr. Pascual said he
could so that appointment was schedule for Friday morning.
Dr. Pascual reviewed the chest X-rays, and the CT scan an explained the next
step which would be a bronchoscopy procedure (link:
http://www.mayoclinic.com/health/medical/IM04196) to go down and look at the
lungs to see what is actually there. If it is something they can grab/remove,
the can do that, if not, they can biopsy it and proceed to the next step. So
that procedure was scheduled for the following Monday, November 2nd.
The findings from that procedure indicate there was some growth in that upper
right-lobe of the lung. It also indicated that the rest of my lungs looked
fine, no issues which was good. After the growth, the indicated it was vascular
in nature, i.e. bloody, so they could not take a chunk biopsy since they would
not want it to start heavily bleed, but did feel comfortable taking a couple
needle biopsies.
Dr. Pascual contacted me on Wednesday to indicate the results. He said that the
biopsies were not conclusive since they were basically just blood. Meaning
there was no cancer in the blood, but since they were not able to get a chunk,
the test is technically inconclusive. He said the next step would be to get a
PET scan to check for cancer in other parts of the body and the schedule a
surgical consult to have that upper right section of the lung removed. He
indicated it might be able to be removed with VATS (Video-Assisted Thoracoscopic
Surgery, link:
http://www.mayoclinic.org/video-assisted-thoracic-surgery), but that would
be up to the surgeon.
The following week I went in for my PET (Positron Emission Tomography, link:
http://www.mayoclinic.com/health/pet-scan/MY00238) scan, of which the
results of that showed that the upper right lobe of the lung was cancer of some
sort, and there were three lymph nodes that also showed a higher metabolism
rate. For the lymph nodes, since they are part of the immune system, that does
not necessarily mean cancer, it could mean infection. But the rest of my body
was clean, so it appeared that all that was needed was to cut out the bad lung
section.
My surgical consult was not scheduled until November 24th, but I
called to check on any cancellations the prior week and was able to see that
doctor on November 17th. The doctor that would be doing the surgery
was Dr. John Odell MD (link:
http://www.mayoclinic.org/bio/11677872.html). During that meeting we
talked about the surgery, the VATS procedure and if he could not do that, the
more invasive type surgery, thoracotomy (link:
http://www.webmd.com/lung-cancer/lung-surgery-thoracotomy-for-lung-cancer),
which is a larger cut and longer recovery time. If VATS could be used, then the
hospital stay would be 3-4 days, if the other, than 5-7 days. Well, in any case
I felt like I was in good hands, Dr. Odell had been doing this surgery for a
couple of decades, and does these 3 or 4 times a week.
At this point they thought it was something called a carsonoid
growth/tumor/cancer (click for a good write up on
this). This a rare type of cancer, slow growing, but once it is
removed all should be fine. Dr. Odell indicated until recently it was not even
considered cancer, but now is classified as cancer, but in the full spectrum of
cancer, this is way on the end of slow growing and normally not something to be
worried about. The most interesting part of the
PDF article I link
to here is on page #4, under "How Are Lung Carcinoid Tumors Diagnosed?"
... "Some patients with central carcinoid tumors may have a cough, may cough up bloody sputum".
Which was my exact situation back in October 2008.
So, my surgery was scheduled of November 23rd. This was incredible
since it was less than 30 days since my annual physical that discovered it.
On Monday, November 23rd I arrived at Mayo for my surgery with my
wife Katie. I went into pre-operation room about 9am where they set up my IVs,
took blood, and hooked up my epidural to my upper back. I believe it was about
10:30 or so when I wheeled me off to the operating room.
Originally Dr. Odell indicated that the surgery (his part) would normally only
take about 1-2 hours. Apparently I was in there for about 3 or so hours. The
reason was once they go into that area Dr. Odell realized that the section of
the lung was worst off that originally believed, it was harder to remove and
kind of adhered itself to the chest wall. He was not able to use the VATS
procedure so there was about a 5-6 inch veridical cut under my right arm where
they accessed my lung. They had to use some rib spreaders to gain further
access.
About 3pm or so he came out to talk Katie about the surgery. He indicated the
surgery went well, but during that conversation his beeper went off and it
indicated he was needed back since my blood pressure was dropping. Apparently I
coughed or something which broke one of the sutures that was one a main blood
vessel. He went back in and for about an hour or so Katie did not know what
that story was, and that was certainly a dark valley for awhile. After about
an hour or so, Dr. Odell came back out to explain that I was doing fine again
and all should be good. I apparently lost about 4 units of blood and was given
blood, but all was okay and I was stable again. He told us later that the last
time that happened to him was like 27 years ago.
I moved me to the ICU unit for Monday and Tuesday. I was pretty much asleep
until Tuesday morning/afternoon. It was Tuesday they removed my breathing
tubes and by Tuesday night I was drinking liquids again. They removed the
urinary catheter on Tuesday evening as well. I still had EKG stuff on my
connected to a remote device, a chest tube to drain excessive fluid from the
cavity, and my epidural line going to my back.
By Wednesday I was feeling much better and was ready to move to a normal room,
but had to stay in ICU since there was no rooms currently available. I was
already eating and stuff.
Each day I had to get a chest X-ray to check on seeing how the cavity area was
doing. On Friday they decided I needed another chest tube, higher up to help
drain additional fluid from that section. So on Friday morning I had an
additional one added.
By Wednesday they had the results back from testing the lymph nodes and them
came back clean. So, with the removal of the one section of lung, that should
do it, no chemo, no radiation, just remove and be done with it.
And as far as the type of cancer, it was not a carsonoid, but rather a
mucoepidermoid carcinoma (link:
http://www.surgical-pathology.com/mucoepidermoid_carcinoma_lung.htm). This
is another type of rare cancer, apparently only about .02% of the total each
year (that’s like 60 cases out of 300,000). But this is a type that could be a
fast growing form of cancer, so I am very happy it was caught early and removed.
Each day I was feeling better, more strength and able to do more walking to
exercise the body and the lungs. When Katie and Ryan visited me on Friday
night, Dr. Rodriguez visited which was very nice.
On Saturday they removed my epidural which was great since it was kind of itchy.
Also each day about 7am, Dr. Odell and his team would come visit to see how I
was doing. On Sunday, November 27th when they came in to check me,
they indicated my fluids were draining slow enough that I could have the tubes
removed and I could go home.
So, Sunday the 27th I got to go home, indicated to return to regular
diet and routine. I took off the next week just to rest and see how I was
doing. I was already feeling about 80% when I left the hospital, and felt
better each day once I got home. A real blessing from God was that I was in
almost no pain, and I was not using any pain medicine. I was using a little
Tylenol for the aches, but almost nothing which was great. By Wednesday I was
feeling about 90% and even went to our church services that night with Ryan.
And I was able to drive myself since I was not on any pain meds that would
prevent me from doing so. I joined Katie and Ryan for our co-op home school
group on Thursday and we went to the Nutcracker on Friday when them. By the
weekend, December 5th, I was feeling about 95% back to normal so I
made the decision to return to work on Monday. So with the exception of just
healing and taking it easy, no heavy lifting, I was doing just great by the 7th.
I go back to see Dr. Odell for a follow-up appointment on December 15th.
And will probably meet with Dr. Pascual which he said I would need to do a
periodic CT scan just to check/verify that nothing else is growing for the next
couple of years.
So, that’s the story.
![]()
God is good!
J
Joe Vogel, 2009
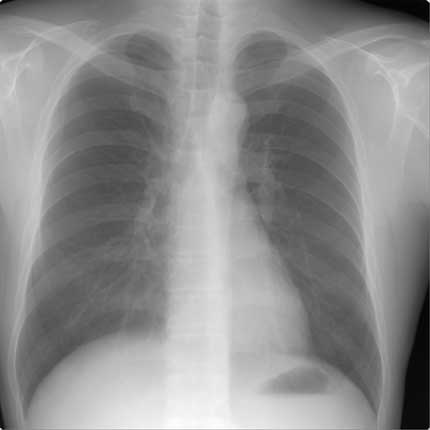
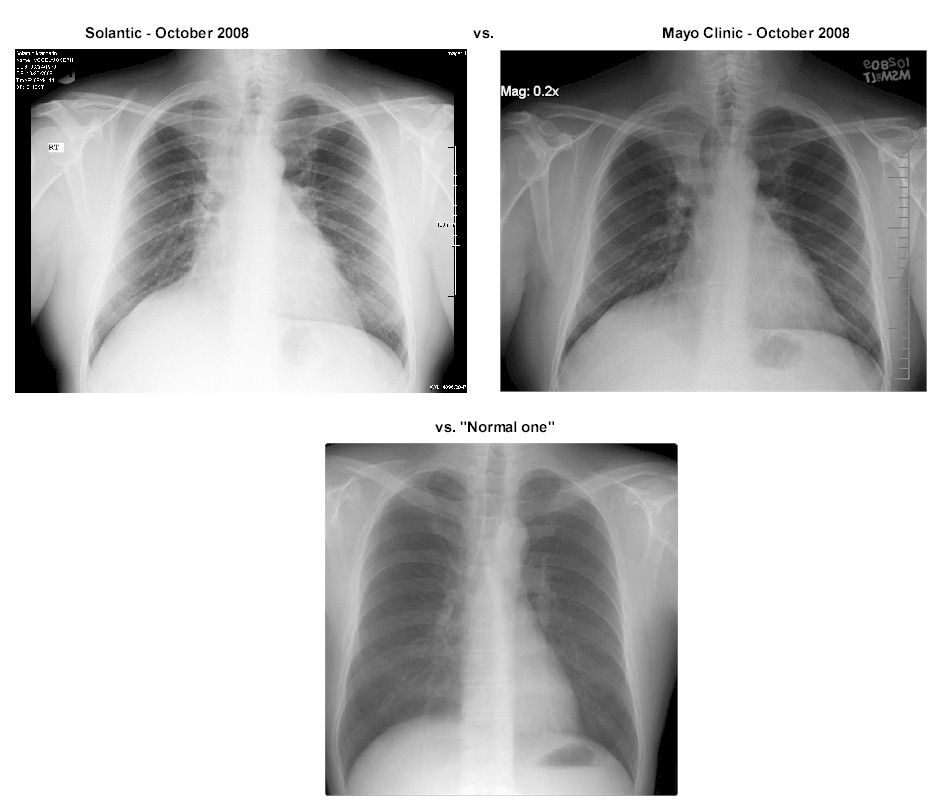
Example of a real "Normal Lung" of a 40-year old male:
X-Ray of my chest done by Solantic and indicated as
"normal lung" in October 2008:
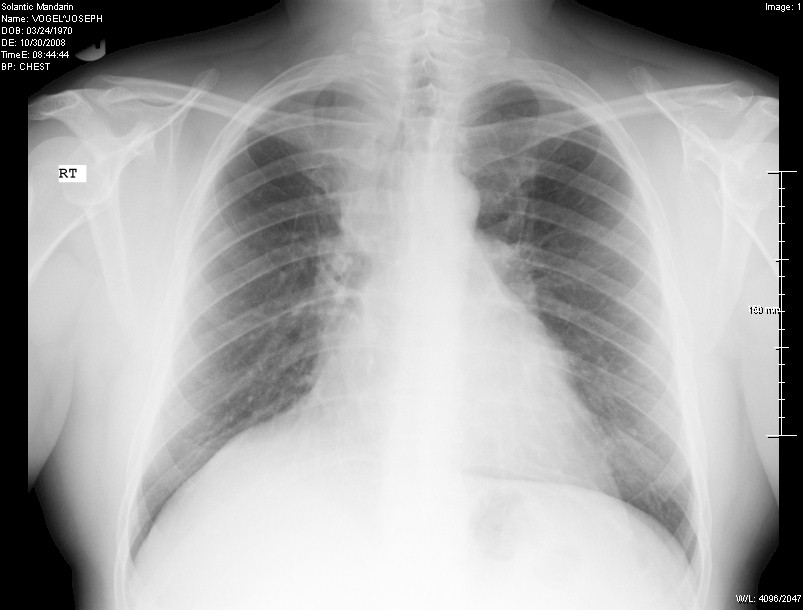
When you compare this to the example of a real normal one above, you can see how
the right side it shifted up and the upper right area is not as dark.
The dark area indicates "air" in the lung (when you get a chest x-ray they ask
you to breath in deep). Also note on the left hand side you see more of a
full lung, remembering that the heart is in front of the lung on that side so it
does not show up as dark.
But you can tell something is not quite right with the right lung presentation.
Nonetheless, the Solantic doctor indicated it as "normal
lung".
X-Ray of my chest done by Mayo and indicated as
"abnormal lung" in October 2009:
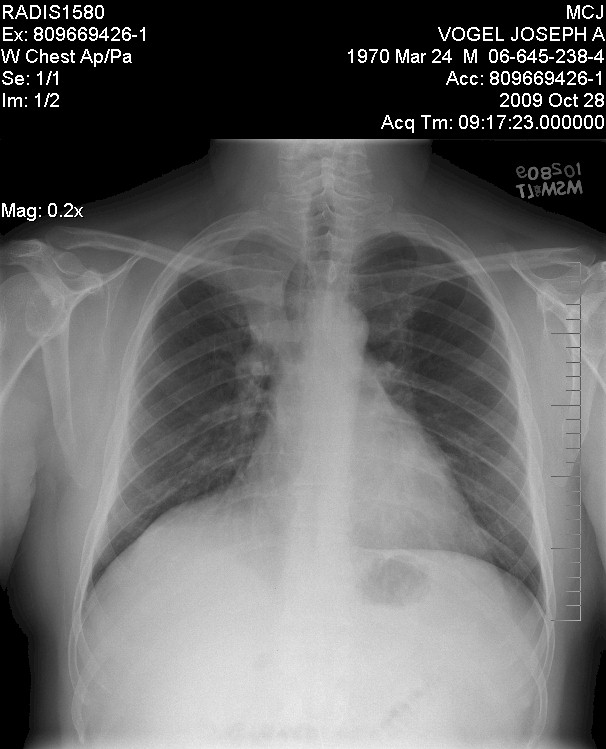
So, as you can see, basically the EXACT same!
Which in one way was good since it had not gotten worse, BUT it was the exact
same so Solantic totally missed it!
Arg!
So, let's compare ....
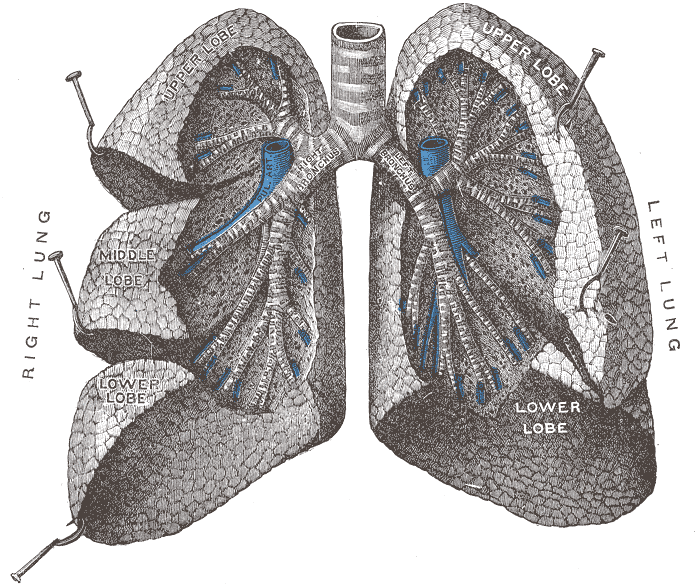
Good
illustration of the lobes of the lung, they removed the upper right (smallest)
lobe on me:
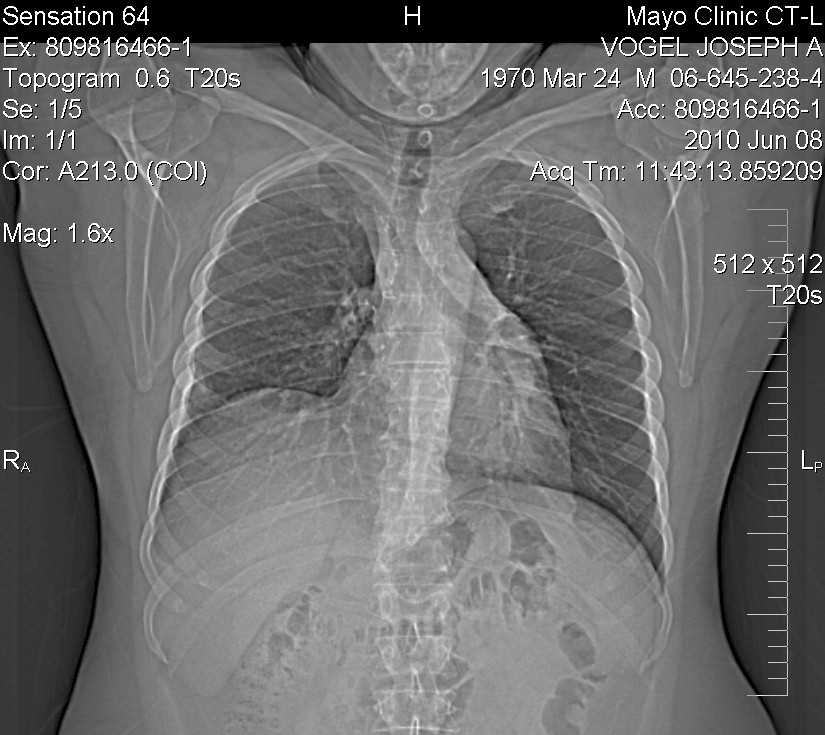
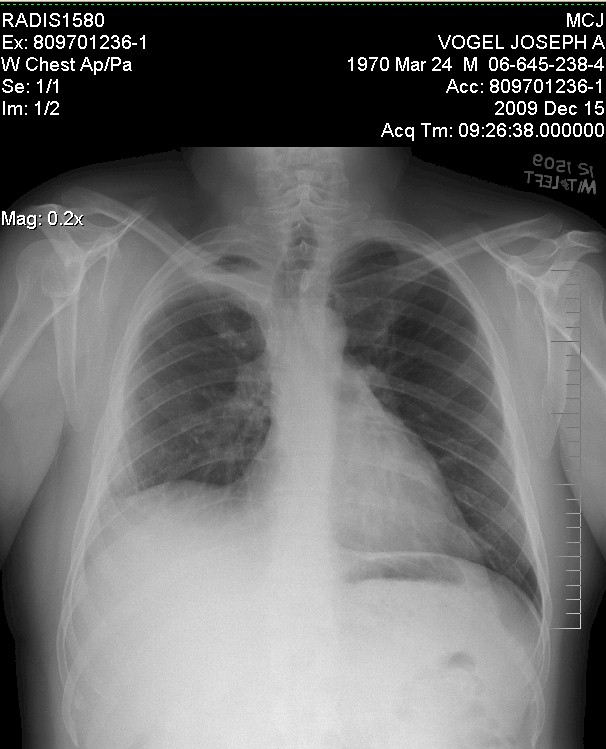
So, as of December 2009, with the upper right lobe of the lung removed, my
current chest x-ray looks like:
As time passes, they say the two remaining lobes might grow in size to since
there is more room, but the doctors say all looks great as of that date.
X-ray on follow-up after surgery/recovery - December 15 2009
CT Scan - 6 months later - June 25th 2010 - Based on
the notes from the scan, all appears good (aka "unremarkable")